
Massage in the Time of Bushfire Crisis
By Tim Clark
Like many, I have watched the Australian bushfires with a sense of helplessness and heartbreak for those affected.
How can we best work with people who may be dealing with huge losses, trauma, anxiety and any number of ongoing stressors?
I’ve thought about some questions that massage therapists might have about working with affected people, and I invite people to add other questions in the comments, especially if you have been working, or are planning to work, in these areas.
Should I bring up the bushfires with my clients?
As a rule of thumb, I wouldn’t recommend raising the topic if your client does not. You’re in a position to offer rest and respite to people whose day-to-day experience may be filled with reminders of the fires. That said, I can imagine there might be situations where it’s like the elephant in the room and not raising it could feel awkward. Your client might notice if you are deliberately avoiding talking about the fires and think they can’t bring it up even though they want to.
Follow your client’s lead. Stay attuned. They may relish the opportunity to talk about it and have their feelings witnessed. Or they may relish the opportunity not to have to think about it at all.
If my client brings it up, what do I say?
You’re not obliged to say much at all. By all means, let your massage do the talking.
If it seems like your client does want to talk about their experience, be empathic:
“That sounds really hard.”
“That’s a lot to deal with.”
And comforting:
“You’re safe here.”
“Good on you for taking this time out for yourself.”
Sympathy is okay too:
“I’m really sad/sorry to hear that.”
– but some people might take that as a sign they’ve brought you down, so keep it brief.
Focus on being warm and accepting and providing a space for your client to feel whatever they are feeling. You don’t have to be upbeat and optimistic, nor do you have to be solemn and morose.

Avoid getting involved in blaming or political discussions. Maybe your client has something they want to get off their chest? Let them, but avoid anything judgemental, even if you’re in agreement. Let it be a time for observation rather than judgement.
Avoid talking about hypothetical fire-related situations e.g. “If you’d stayed…”, “If you’d done things differently…”) and definitely don’t ask “Were you insured?” The last thing you want is your client lying on the table wondering about whether they made the right decisions under life-threatening conditions.
What advice do I give my clients?
Be aware they may well be getting all sorts of advice from all sorts of people. Don’t feel obliged to add to it. If it feels appropriate, encourage clients to keep up their self-care and their social connections, e.g. talking to trusted friends and relatives.
Therapists might want to print up copies of this information sheet from the Australian Psychological Society that outlines self-care strategies for bushfire recovery. (They’re good for therapists too!)
What if my client gets upset at some stage during the treatment?
Do what you would normally do (check in, offer a break if necessary), but you may need to be a little more attuned than usual. It might be the first time in a while your client has felt safe enough to ‘let their guard down’ and emotions can spill over. As much as possible, just let your client feel what they are feeling, without trying to move it or fix it.
Show support through actions, rather than words.
Offer tissues, water, tea or whatever is appropriate, but don’t offer hollow reassurances such as “It’ll all be okay”, which can sound like you’re minimising the immense challenges your client may need to face before normality returns.
What if it seems like your client is traumatised or at-risk?
Keep an eye out for trauma symptoms. Watch particularly for clients who tell you they are having:
- Recurrent intrusive and unwanted thoughts or flashbacks
- Difficulties with concentration
- Ongoing sleep problems
- Persistent irritability
- Prolonged feelings of anxiety.
If you think the client may have trauma that has gone unrecognised: refer, refer, refer.
Details about government-funded mental health services for bushfire recovery can be found here.
Always remember your boundaries and scope of practice: they are there to protect both you and your client.
Keep the following list of numbers handy and pass them on to clients if you suspect they are depressed, suicidal or otherwise at-risk:
- Lifeline on 13 11 14
- beyondblue on 1300 224 636
- MensLine Australia on 1300 789 978
- Suicide Call Back Service on 1300 659 467
- Kids Helpline on 1800 551 800
- Headspace on 1800 650 890
- QLife on 1800 184 527
Should I change anything about how I massage these clients?
As always, check your client’s preferences before the massage. Give them plenty of autonomy and choice in how the massage goes. They may have had a string of recent experiences that have robbed them of choice. You have an opportunity to re-empower them, even in this small way.
Be aware that your client may be experiencing hyperarousal or hypervigilance. Their nervous system may be set permanently to alert because they have experienced a life-threatening situation. Living in hyperarousal for a prolonged period can cause severe fatigue. Vigorous or sudden applications of pressure may exacerbate symptoms of fatigue and cause muscles to guard rather than relax.
Try instead to move your client from sympathetic (fight-or-flight) to parasympathetic (rest-and-digest) dominance by using a regular rhythm, long, slow strokes and moderate, even pressure. You might encourage your client to focus on their breath, counting 4 in and 6 out, to further relax the nervous system and quieten the mind.
How long will the effects of the bushfires last?
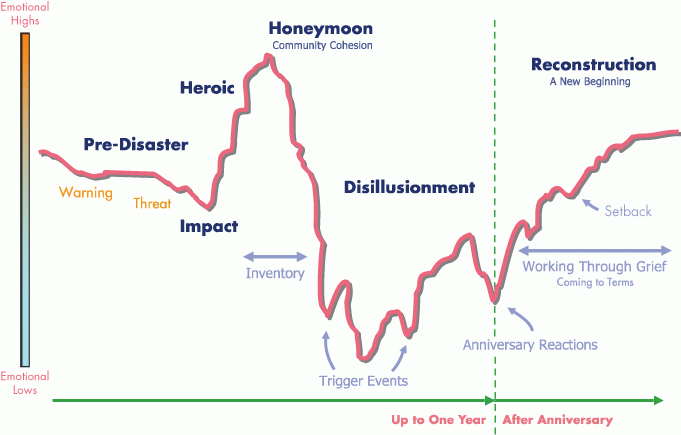
Recovery, including emotional recovery, from disasters like these takes a long time. Generally, the most difficult time for people will be when it feels like the public interest has died down but the challenges remain, and disillusionment sets in. It may well be about three years before life returns to a sense of normality and stability, perhaps longer. Anniversaries of the event can be particularly difficult during the recovery phase.
This diagram gives an idea of a typical trajectory of the emotional recovery process. Notice that the lowest point is not (necessarily) the impact of the disaster itself but the depths of disillusionment.
We always need to remember that everyone has their own way of recovering. There’s no right or wrong way to do it.
What if I find myself getting upset, depressed or exhausted?
Take your own self-care seriously and be a model of self-care for others.
Be realistic about your limits. Don’t expect perfection. It’s admirable to want to do as much as you can but exhausting or traumatising yourself isn’t only risky for you; it also puts your clients at risk.
You are not responsible for making everyone feel better. You have an opportunity to contribute what you reasonably can to a very big problem. That is all anyone expects of you. It might feel small or inconsequential but for the people you treat it will be a huge gift.
Listen to your body. If it’s telling you you’re tired, stop, even if only for half an hour. If you ignore your body, it will find its own way to make you stop. Watch for signs of burnout such as:
- Resentment
- Cynicism
- Catastrophic thoughts
- Social withdrawal
- Absence of positive emotions.
If you are in a situation where you are regularly treating bushfire victims, start by taking precautions such as spacing out your treatments to include substantial breaks, limiting the length and number of treatments you do in a day, and having a trusted friend or colleague to regularly debrief with, especially if you notice feeling emotionally triggered.
Trauma is contagious. Just hearing stories of trauma can be traumatic and, if you’re hearing them on a regular basis, the effects of trauma can accumulate. This often happens outside our awareness and we only know it has happened when we find ourselves broken down and unable to continue.
Build pleasurable activities into your day in a deliberate way. Set aside time to read a book, listen to music, go for a walk or play a game. Find someone to do a massage swap with. Be disciplined about it.
As long as we can do it in a way that keeps everyone safe – ourselves included – we have a wonderful opportunity to make life easier, happier and better for people who have experienced great hardship. It’s what we do!
About the Author

Tim Clark is a massage therapist and psychotherapist in private practice in Melbourne’s south-east. His research paper, ‘The Psychotherapeutic Relationship in Massage Therapy’ was published last year in the International Journal of Therapeutic Massage and Bodywork. You can read it here.




Christine Knox
22/01/2020 - 5:02 pm
Thank you for your article – a measured, compassionate commonsense approach to helping others whilst looking after yourself too.
Tim Clark
23/01/2020 - 10:00 pm
Glad you thought so Christine! Thank you for your comment.
Ronna Moore
25/01/2020 - 3:45 pm
Hi Tim
Thank you for this sensible and helpful post. I value all your observations. And I could do with one of those beautifully described massages right now!
I am inclined, though, just to take a slightly different tack than the one you described at the outset of your piece. Working from the premise that trauma, loss and grief are mind-body phenomena, I feel that as body workers, we have an opportunity to be more proactive in this space.
As a result of the widespread and ongoing nature of the bushfire crisis, it appears that there is an equally widespread level of alert throughout the general population, whether or not people have been directly impacted. So from this point of view, with every client/patient I am currently seeing, I do ‘check in’ specifically (although gently and mindfully) with how people are travelling with respect to the fires. And for a number of reasons.
1. I see this as an opportunity to provide ‘somatic education’ about common physical responses to grief and loss. (It is very interesting how many people are surprised that there are multiple, common physical manifestations of grief and loss. In my experience, it can be profoundly reassuring (and empowering to some extent) for people to know that generalised muscle discomfort or agitation, fatigue, headache, gut disturbance, tachycardia, an escalation of preexisting pain and so on may be the consequence of trauma anxiety and grief. (Oh, right, that may explain it…maybe I am not going crazy…maybe I am not coping as well as I thought…maybe I do need to take care, seek some help with this……that’s interesting, I will watch out for that….) I see such information sharing as being part of our remit (and within our scope of practice), just as we provide other information relating to physical well-being. Such information sharing can be seen as similar to the provision of psycho-education by psychologists or counsellors. It is not diagnosing or counselling, it is resourcing and it sits alongside the provision of fact sheets, encouragement to seek additional support and to actively refer (as in the circumstances you have carefully identified). I see this as our role as engaged health professionals.
2. Whatever the presenting issue is, there may be the potential for either background or acute stress arising from the fires to serve as an exacerbating factor. For example, the impact of stress on pain. This is actually no more than I normally do, “So, what is happening in your life right NOW which might be having an impact on…..” but I am being particularly mindful about the fire situation. It may change the approach to treatment…..
3. There is good evidence to support massage therapy as an ‘intervention’ for modulation of anxiety (and to some extent, trauma) and we need not be afraid to be upfront about this. For example, if referring to a grief counsellor, psychologist or GP, I am recommending a referral back to me for ongoing ‘body’ therapy for the reasons you articulated that we are good at….facilitating safety (and encouraging, in the process, a multi-disciplinary approach to care). And BTW a big shout out to Bessel van der Kolk and others here for recognition of the role for massage therapy in trauma recovery.
I would be interested in your thoughts about above, Tim.
And, just one other thing….. I think as MTs, we can tend to assume that down regulation of sympathetic activity is helpful. But in my reading of the literature, (and personal experience) stress and trauma can also lead to hypo-activation of the para-sympathetic system…..this will be the person with very flat affect, fatigue, listlessness, maybe bradycardia….maybe also unlikely to attend for massage therapy (!), except that I have had exactly this circumstance arise….
Thanks again Tim for your great article. I have banged on a bit because I feel it is an important moment for massage therapy to make a valuable contribution.
Tim Clark
26/01/2020 - 12:36 pm
Thank you so much for all of this Ronna. I’m so glad that you’ve taken the time to add to the discussion, as I only really envisioned my piece as being a starting point, in the knowledge that hearing how someone else (i.e. me) would do things can sometimes serve to clarify for us how DIFFERENTLY we would do things.
I think you’ve highlighted the impossibility of writing a ‘guide’ or ‘list of rules’ for things like this that is going to work for every therapist and every client. There are so many ‘mights’ and ‘maybes’ in my piece that I almost questioned the value of writing it in the first place! I really saw much of what I wrote as a list of options, rather than hard and fast laws, and certainly not as the last word on the topic.
It’s clear to me just how much my personal style of communication – which is at times passive to a fault – has influenced what I’ve written, inevitably I guess. I love your proactive approach and can see tons of value in it for helping clients to better understand what they’re feeling. There are clients for whom it would be an absolute gift. And I totally agree with you about it not being ‘diagnosing’ or ‘counselling’.
My guiding question is always “What’s in the best interests of the client?” Somatic education may be absolutely appropriate, but I guess I do keep that ‘may be’ in mind, just as I would with psychoeducation for my counselling clients. That sort of education is most helpful when the client is ready to take it on board. I’ve had clients for whom the idea of the mind-body connection is totally new and just feels too ‘out there’, and all the evidence in the world won’t sway them, at least not until we’ve had time to establish a trusting relationship. So I guess that’s part of the thinking behind my kind of ‘one-client-at-a-time’ approach.
I love your approach to referral, and would absolutely do that if the client and I were in a position to be able to. That’s a beautiful way to truly support the client in a holistic way.
And I totally agree with you that we need to keep hypo-arousal in mind. Again, I think it’s a ‘one-client-at-a-time’ thing. Hypo-arousal would call for a different mindset for treatment, but it’ll depend on what else might be happening for the client (i.e. pain, depression, fatigue) as to how it would impact the massage itself.
It brings to mind a lovely thing Deb Dana wrote about touch in her book on Polyvagal Theory (which is admittedly aimed at psychotherapists): “What kind of touch is an effective regulator? What kind of touch predictably dysregulates? … The answers to these questions will be different for each client.”
And I’ll add three more cheers for BVDK!
Thank you again for pushing the discussion along. (You should definitely consider writing for the blog in future. I was planning to write a follow-up piece on working with clients experiencing climate-related anxiety and trauma generally…but I’d much rather hear someone else’s thoughts on the topic…)
Ronna Moore
30/01/2020 - 7:03 am
Hi Tim
Thank you again for your observations. I completely agree with you in ‘meeting clients where they’ are….and a careful dance from there.
BVDK is here soon, any chance that you will be there?
Learning about others’ thoughts and approaches is nourishment…..
(And thank you for encouragement re blog….I have contributed in the past).